| Issue |
Parasite
Volume 27, 2020
|
|
|---|---|---|
| Article Number | 27 | |
| Number of page(s) | 19 | |
| DOI | https://doi.org/10.1051/parasite/2020025 | |
| Published online | 30 April 2020 | |
Review Article
Cryptosporidiosis in HIV-positive patients and related risk factors: A systematic review and meta-analysis
Cryptosporidiose chez les patients VIH-séropositifs et facteurs de risque associés : revue systématique et méta-analyse
1
Research Center for Evidence Based Medicine (RCEBM), Tabriz University of Medical Sciences, 5166-15731 Tabriz, Iran
2
Student Research Committee, Tabriz University of Medical Sciences, 5166-15731 Tabriz, Iran
3
College of Veterinary Medicine, South China Agricultural University, 510642 Guangzhou, China
4
Department of Parasitology and Mycology, Faculty of Medicine, Mashhad University of Medical Sciences, 91779-48964 Mashhad, Iran
5
Iranshahr University of Medical Sciences, 99147-86138 Iranshahr, Iran
6
Clinic for Infectious and Tropical Diseases, Clinical Centre of Serbia, 11000 Belgrade, Serbia
7
University Lyon, ICBMS UMR 5246 CNRS-INSA-CPE & Institute of Parasitology and Medical Mycology, Croix-Rousse Hospital, Hospices Civils de Lyon, 69004 Lyon, France
8
Center for Health Related Social and Behavioral Sciences Research, Shahroud University of Medical Sciences, 36147-73947 Shahroud, Iran
9
Department of Biomedical Sciences, University of Sassari, 07100 Sardinia, Italy
10
Department of Parasitology and Mycology, Faculty of Medicine, Tabriz University of Medical Sciences, 5166-15731 Tabriz, Iran
11
Immunology Research Center, Tabriz University of Medical Sciences, 5166-15731 Tabriz, Iran
12
Drug Applied Research Center, Tabriz University of Medical Sciences, 5166-15731 Tabriz, Iran
13
Infectious and Tropical Diseases Research Center, Tabriz University of Medical Sciences, 5166-15731 Tabriz, Iran
* Corresponding authors: This email address is being protected from spambots. You need JavaScript enabled to view it.
, This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
1
October
2019
Accepted:
9
April
2020
Abstract
Cryptosporidium is one of the major causes of diarrhea in HIV-positive patients. The aim of this study is to systematically review and meta-analyze the prevalence of Cryptosporidium in these patients. PubMed, Science Direct, Google Scholar, Web of Science, Cochrane and Ovid databases were searched for relevant studies dating from the period of 1 January 2000 to 31 December 2017. Data extraction for the included studies was performed independently by two authors. The overall pooled prevalence was calculated and subgroup analysis was performed on diagnostic methods, geographical distribution and study population. Meta-regression was performed on the year of publication, proportion of patients with diarrhea, and proportion of patients with CD4 < 200 cells/mL. One hundred and sixty-one studies and 51,123 HIV-positive participants were included. The overall pooled prevalence of Cryptosporidium infection in HIV-positive patients was 11.2% (CI95%: 9.4%–13.0%). The pooled prevalence was estimated to be 10.0% (CI95%: 8.4%–11.8%) using staining methods, 13.5% (CI95%: 8.9%–19.8%) using molecular methods, and 26.3% (CI95%: 15.0%–42.0%) using antigen detection methods. The prevalence of Cryptosporidium in HIV patients was significantly associated with the country of study. Also, there were statistical differences between the diarrhea, CD4 < 200 cells/mL, and antiretroviral therapy risk factors with Cryptosporidiosis. Thus, Cryptosporidium is a common infection in HIV-positive patients, and safe water and hand-hygiene should be implemented to prevent cryptosporidiosis occurrence in these patients.
Résumé
Cryptosporidium est l’une des principales causes de diarrhée chez les patients séropositifs pour le VIH. Le but de cette étude est de revoir et méta-analyser systématiquement la prévalence de Cryptosporidium chez ces patients. Les bases de données PubMed, Science Direct, Google Scholar, Web of Science, Cochrane et Ovid ont été recherchées pour des études pertinentes datant du 1er janvier 2000 au 31 décembre 2017. L’extraction des données pour les études incluses a été réalisée indépendamment par deux auteurs. La prévalence globale combinée a été calculée et une analyse en sous-groupes a été effectuée sur les méthodes de diagnostic, la répartition géographique et la population étudiée. Une méta-régression a été réalisée pour l’année de publication, la proportion de patients atteints de diarrhée et la proportion de patients avec CD4 < 200 cellules/mL. Cent soixante et une études et 51,123 participants séropositifs ont été inclus. La prévalence globale combinée de l’infection à Cryptosporidium chez les patients VIH-séropositifs était de 11,2 % (IC95 % : 9,4 %–13,0 %). La prévalence regroupée a été estimée à 10,0 % (IC95 % : 8,4 %–11,8 %) en utilisant des méthodes de coloration, 13,5 % (IC95 % : 8,9 %–19,8 %) en utilisant des méthodes moléculaires et 26,3 % (IC95 % : 15,0 %–42,0 %) en utilisant des méthodes de détection d’antigènes. La prévalence de Cryptosporidium chez les patients infectés par le VIH était significativement associée au pays d’étude. En outre, il existe des différences statistiques entre la diarrhée, les CD4 < 200 cellules/mL et les facteurs de risque du traitement antirétroviral avec la cryptosporidiose. Ainsi, Cryptosporidium est une infection courante chez les patients séropositifs, et une eau salubre et une hygiène des mains doivent être mises en œuvre pour prévenir la survenue de cryptosporidiose chez ces patients.
Key words: Cryptosporidium infection / HIV / AIDS / Systematic review
Ehsan Ahmadpour and Hanie Safarpour contributed equally to the article.
© E. Ahmadpour et al., published by EDP Sciences, 2020
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Cryptosporidium is an intracellular protozoan parasite that infects the gastrointestinal epithelium of a wide range of animals as well as humans, and causes diarrheal disease [29, 103]. Among the 38 species of Cryptosporidium currently recognized, Cryptosporidium hominis and Cryptosporidium parvum are responsible for the majority of human infections [43]. However, other species including C. meleagridis, C. canis, C. felis, and C. muris have been identified in immunocompromized patients [178]. Transmission of the infection is most common by the fecal-oral route, via the consumption of contaminated water and food, and contact with infected persons or animals [29]. Infection in immunocompetent patients is either asymptomatic or presents with profuse acute or persistent watery diarrhea, nausea and vomiting, stomach cramps, and occasionally fever that lasts approximately 2 weeks. However, in patients with immune deficiencies, the infection might cause prolonged symptoms and lead to chronic diarrhea that lasts more than 2 months, or fulminant diarrhea with more than 2 L of watery stools per day [29].
It is estimated that in 2016, 36.7 million people were infected with HIV worldwide. During the onset of the AIDS epidemic in the early 1980s Cryptosporidium became widely recognized as a human pathogen [160]. Diarrhea is a common problem in AIDS patients and about 30%–60% of patients in developed countries and 90% in developing countries experience diarrhea [44]. Diarrhea significantly influences quality of life and can lead to complications such as dehydration, malnutrition, weight loss and even death [101]. Cryptosporidiosis was considered one of the original AIDS-defining illnesses and a major risk factor for mortality compared to other AIDS-defining illnesses [32]. The prevalence of Cryptosporidium in immunocompetent patients varies widely, ranging from 0% to 10%, depending on country socioeconomic status [28]. Several studies have investigated the prevalence of Cryptosporidium in HIV-positive patients and have reported a wide range of estimates in different settings.
The aim of the study was to systematically review and meta-analyze the worldwide prevalence and geographic distribution of Cryptosporidium in HIV-positive patients and to compare the estimated prevalence using different diagnostic methods.
Methods
Search strategy and study selection
We performed this systematic review and meta-analysis according to the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) statement [87]. PubMed, Science Direct, Google Scholar, Web of Science, Cochrane and Ovid databases were searched from 1 January 2000 to 31 December 2017 restricted to the English language using the following keywords: “Cryptosporidium”, “cryptosporidiosis”, “HIV”, “immunodeficiency”, “acquired immune deficiency syndrome”, or “AIDS”. After removing duplicate records, two authors independently reviewed the titles and/or abstracts of all records identified by the search. Full-texts were retrieved and evaluated for potentially relevant studies. All disagreements were resolved by consensus.
Inclusion and exclusion criteria
Studies were included in the systematic review and meta-analysis if the study was performed on HIV/AIDS patients with or without diarrhea and the prevalence of Cryptosporidium was evaluated using staining, antigen detection or molecular methods. Conference abstracts, animal studies, case reports, comments, and reviews were excluded. When duplicate reports of the same research were suspected, the paper reporting more relevant data was included.
Data extraction
Data extraction was performed independently by two authors and the following information was extracted: first author, year of publication, country of study, average level of income in the country of study, region of study, study design, number of HIV/AIDS participants, sex ratio of participants, mean age, diagnostic methods, number of participants co-infected with Cryptosporidium, number of participants with CD4 counts < 200 cell/mm3, and number of participants with diarrhea. The region of study was determined according to the WHO Global Burden of Disease Regions [176]. The level of income was retrieved from the 2017 World Bank classification of countries by income [175].
Meta-analysis
Comprehensive meta-analysis 2.2 (Biostat Inc., USA) was used to calculate the pooled prevalence using a random-effects model. Heterogeneity was assessed using the I2 index and Cochran-Q test. An I2 index >70% or a significant Cochran-Q test indicated heterogeneity [37]. Also, publication bias was assessed using Egger’s intercept and visual inspection of the funnel plot. Univariate analysis was performed on the following risk factors and variables: diagnostic method, country of study, average level of income in the country of study, region of study, number of participants >100, proportion of patients with diarrhea, and proportion of patients with low CD4 counts. Meta-regression was performed using the method of moments on the following variables: year of publication, the proportion of patients with diarrhea, and proportion of patients with low CD4 counts.
In all analyses, if a study used multiple diagnostic methods, we preferred the prevalence estimated using molecular methods to the other two, and staining methods to antigen detection methods. This procedure was implemented for all analyses except in the subgroup analysis of diagnostic methods. In these studies, all estimates of prevalence using different diagnostic methods were included. Publication bias was assessed using Egger’s regression and visual inspection of the Funnel plot. A significant Egger’s regression and an asymmetric Funnel plot indicated publication bias [37]. The level of significance for all tests was p < 0.05.
Results
Search results
After removing duplicates, titles and/or abstracts of 1986 records retrieved by the search were screened and 237 studies were selected to be reviewed in more detail using their full-texts. Of these, 161 studies fit the inclusion criteria and were included in the systematic review and meta-analysis (Fig. 1).
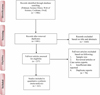 |
Figure 1 Flowchart describing the study design. |
Characteristics of studies
A total of 51,123 HIV/AIDS patients participated in these studies of which 5408 patients were co-infected with Cryptosporidium. The overall male to female ratio was 61.2% to 38.8% (M:F = 1.58:1) among all participants and 67.2% to 32.3% (M:F = 2.08:1) among infected participants. The mean age of participants in the included studies was 33.9 years (ranged from 10 months to 45 years). In total, studies from 40 countries worldwide were included. The countries with the most included studies were India (25%, 41/161), Ethiopia (11%, 18/161), Brazil (8%, 12/161), Nigeria and Iran (6%, 10/161). More than 40% of studies were performed in lower middle-income countries (68/161), followed by upper-middle-income countries (32%, 52/161), low-income countries (20%, 33/161) and only 5% were performed in high-income countries (8/161). Studies were also categorized based on the WHO Global Burden of Disease Regions with 33% (53/161) of studies coming from the African region, 6% (10/161) from Eastern Mediterranean countries, 3% (5/161) from the European region, 14% (23/161) from the Americas, 34% (53/161) from the South-East Asian region, and 11% (17/161) from the Western Pacific region. In terms of study design, 80% (128/161) of studies were cross-sectional, 12% (20/161) were a cohort, 7% (12/161) were case-control, and one was a case-series. Staining, antigen detection, and molecular methods were used to diagnose Cryptosporidium infection in 87% (140/161), 12% (19/161), and 17% (28/161) of studies, respectively (Table 1). Some of the studies used several methods at the same time to confirm presence of Cryptosporidium.
Baseline characteristics of the included studies.
Statistical analysis
The overall pooled prevalence of Cryptosporidium infection in HIV-positive patients was 14.42% (CI95%: 12.61%–16.32%). Substantial heterogeneity with an I2 of 96.4% and a significant Cochran-Q test was observed. Different diagnostic methods were utilized to detect Cryptosporidium infection which significantly influenced the estimated prevalence (p < 0.05). The pooled prevalence was estimated to be 11.9% (CI95%: 10.2%–13.7%) using staining methods, 16.5% (CI95%: 11.1%–22.8%) using molecular methods, and 35.5% (CI95%: 21.3%–51.2%) using antigen detection methods (Figs. 2–4). The country of studies significantly affected the estimated pooled prevalence (p < 0.05). South Africa had the highest prevalence (57.0%, CI95%: 24.4%–84.5%), while Denmark had the lowest prevalence (1.0%, CI95%: 0.1%–7.0%), although very few studies were performed in these countries. Among countries where more than ten studies were included, India had the highest prevalence (14.1%, CI95%: 10.5%–18.7%), while Brazil had the lowest prevalence (5.4%, CI95%: 2.5%–11.6%). The geographical distribution of Cryptosporidium and HIV co-infection is shown in Figure 5.
 |
Figure 2 Forest plot diagram: The estimated pooled prevalence of Cryptosporidium infection in people with HIV infection by random-effect meta-analysis in included studies based on the PCR technique (first author, year of publication, and country). Note: The area of each square is proportional to the study’s weight in the meta-analysis, and each line represents the confidence interval around the estimate. The diamond represents the pooled estimate. |
 |
Figure 3 Forest plot diagram: The estimated pooled prevalence of Cryptosporidium infection in people with HIV infection by random-effect meta-analysis in included studies based on serological methods (first author, year of publication, and country). Note: The area of each square is proportional to the study’s weight in the meta-analysis, and each line represents the confidence interval around the estimate. The diamond represents the pooled estimate. |
 |
Figure 4 Forest plot diagram: The estimated pooled prevalence of Cryptosporidium infection in people with HIV infection by random-effect meta-analysis in included studies based on the staining method (first author, year of publication, and country). Note: The area of each square is proportional to the study’s weight in the meta-analysis, and each line represents the confidence interval around the estimate. The diamond represents the pooled estimate. |
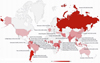 |
Figure 5 Pooled prevalence of Cryptosporidium in HIV-positive patients in different countries (source of image: https://commons.wikimedia.org/wiki/File:BlankMap-World.svg). |
The prevalence in high-income countries was 4.1% (2.4%–6.9%), which was significantly lower than in countries with lower income (p < 0.05). However, no significant difference was observed between upper-middle, lower-middle and low-income countries (p = 0.43). Additionally, the prevalence was not significantly different across WHO Global Burden of Disease Regions (p = 0.46). The South-East Asia region, with a pooled estimate of 12.7% (CI95%: 9.7%–16.4%), had the highest prevalence. Studies including less than 100 participants reported a significantly higher prevalence (15.4%, CI95%: 11.8%–19.8%) compared to the studies with more than 100 participants (8.9%, CI95%: 7.2%–11.0%). The proportion of participants with diarrhea was reported in 42% (69/161) of studies. Additionally, meta-regression showed there is no statistically significant difference within prevalence rate, depending on the year of publication (β intercept = −0.013, p = 0.50). All subgroup meta-analyses were significantly heterogeneous (Table 2). Among these studies, meta-analysis showed that the proportion of participants with diarrhea and CD4 counts < 200 cells/mL significantly correlated with the pooled prevalence (p < 0.0001). Similarly, the proportion of participants who received ART significantly correlated with the pooled prevalence (p < 0.0001) (Table 3). Our study indicated that having diarrhea and having less than 200 CD4 cells μL, in HIV-infected patients, increase the risk of infection by Cryptosporidium, whereas using antiretroviral therapy in HIV-infected patients meaningfully decreases the risk of cryptosporidiosis. The funnel plot showing an asymmetric plot with studies missing on the right side and a statistically significant Egger’s regression suggest the possibility of publication bias (Fig. 6).
 |
Figure 6 Funnel plot of standard error by logit event rate to assess publication or other types of bias across prevalence studies. |
Pooled prevalence of Cryptosporidium in HIV-positive patients and subgroup analyses.
Risk factors associated to Cryptosporidium infection in HIV patients.
Discussion
Diarrhea caused by opportunistic intestinal protozoa is a common problem in HIV-infected patients. With a total number of 36 million HIV-infected patients and 11.2% prevalence of Cryptosporidium co-infection with HIV, approximately 4 million HIV patients are estimated to be infected with Cryptosporidium worldwide. The present meta-analysis of 161 studies published from 2000 to 2017 on the topic of Cryptosporidium infections in patients with HIV shows that the pooled worldwide prevalence of Cryptosporidium in patients with HIV is 14.4%. A systematic review previously assessed the worldwide prevalence of Cryptosporidium among patients with HIV, but did not establish the risk factors [170]. The prevalence of Cryptosporidium in the immunocompetent population has been estimated to be not more than 1% in high-income and 5%–10% in low-income countries [28]. In a case-control study, it was shown that HIV-positive patients had a 20-fold risk of becoming infected with Cryptosporidium [97, 98]. Therefore, in addition to a greater risk of developing symptomatic disease and having more severe and prolonged symptoms, patients with HIV have a greater risk of infection with Cryptosporidium [60].
Several mechanisms have been suggested to explain the susceptibility of AIDS patients to cryptosporidiosis. CD4 cells play a major role in the immune response to gastrointestinal pathogens, and it has been shown that low CD4 counts are associated with increased risk of infection with enteric parasites and chronic diarrhea [104]. Due to immunosuppression, symptoms of cryptosporidiosis in patients with AIDS are expressed differently in terms of severity, duration, and responses to drug treatment. It has been shown that there is a significant relationship between increased mortality rates and cryptosporidiosis in AIDS patients [19, 179]. Similarly, in the present meta-analysis, we showed that the patients with low CD4 counts had a higher prevalence rate of Cryptosporidium infection (p < 0.0001). It seems that IFN-γ is associated with T-cell memory and is a critical regulator of both innate and adaptive immune responses against Cryptosporidium infection. Also, the findings of immunological research suggest that Cryptosporidium induced an inflammatory response in intestinal epithelial cells. Accordingly, the higher expression of inflammatory and pro-inflammatory cytokines, such as CXCL-10 and substance P is present in AIDS patients (compared to AIDS patients without cryptosporidiosis or negative controls) [116]. The opportunistic parasites Cryptosporidium spp. are not only associated with the immune state in HIV-infected patients, but are also more evident with antiretroviral therapy. Utilization of chemoprophylaxis could increase the immunity of HIV-positive individuals and reduce the infection. Our findings suggested that in HIV-infected patients, especially with low CD4 counts, ART should be prescribed.
Substantial heterogeneity was observed between the studies included in this meta-analysis. In addition to using the random effects model, which incorporates some of this heterogeneity, we investigated possible causes of heterogeneity and compared the estimated prevalence in different subgroups and settings [37]. The diagnostic method that was used to detect Cryptosporidium infection significantly influenced the estimated prevalence. The included studies had utilized three main categories of diagnostic methods. PCR is considered the gold standard in diagnosing Cryptosporidium infection with an excellent sensitivity of 97% and specificity of 100%, but is not commonly used due to its high cost and high expertise requirement, especially in low-income countries [28]. The estimated pooled prevalence using PCR was 16.5%, which could be considered as the “real” prevalence. Conventional microscopy, most commonly using Ziehl-Neelsen staining, is an inexpensive and widely available method but has a low sensitivity of 75% [27]. The estimated pooled prevalence using staining methods was 11.9%, which was the lowest estimate among used diagnostic methods. Enzyme Immunoassays (EIA), based on detection of Cryptosporidium antigens, cost more than the staining methods and have a moderate to high diagnostic accuracy, with a sensitivity of 75%–93%. However, confirmatory testing has been suggested when using EIA, since some false-positive reactions have been confirmed [27, 28, 172]. The pooled prevalence using antigen detection methods was the highest among diagnostic methods with an estimate of 35.5%. In addition to false-positive reactions, we propose that the higher prevalence in studies that utilized EIA methods could be due to possible continued shedding of Cryptosporidium antigens in the stools, even after the resolution of infection, although this effect has not been studied.
The geographical distribution was another confounding factor. The estimated prevalence within countries was in a range of 1% in Denmark to 57% in South Africa. Among the countries with more than ten included studies, India (14.1%), Iran (11.1%) and Nigeria (10.6%) had the highest prevalence. The economic status of different countries could be the most probable explanation for these findings. The prevalence in high-income countries, with an estimate of 4.1%, was significantly lower than in middle and low-income countries, but there was no statistically significant difference between the estimated prevalence in the middle-income and low-income countries. Additionally, the source of drinking water can contribute to the different prevalence observed within different countries. A meta-analysis showed that drinking unsafe water significantly increases the risk of Cryptosporidium infection [53]. However, we were unable to evaluate its effect on prevalence since very few studies reported the sources of drinking water. Our study showed that the pooled prevalence across WHO Global Burden of Disease regions was not significantly different.
The association of Cryptosporidium prevalence and the proportion of symptomatic HIV patients has been investigated. No statistically significant difference was observed between the prevalence in studies with a high proportion of symptomatic patients and studies with a low proportion of symptomatic patients, although the meta-regression showed a correlation between prevalence and the proportion of symptomatic patients. Another significant confounding variable was the number of participants in the included studies. Studies with a lower number of participants reported higher prevalence rates. This could be due to the fact that lower sample sizes are associated with higher sampling error [133].
The studies also differed in the period when they were conducted, but meta-regression showed that the year of publication did not correlate to estimated prevalence. A meta-analysis suggested seasonality in the prevalence of Cryptosporidium, and showed that precipitation and temperature are strongly associated with the rate of infection [66]. However, it was not possible to investigate the impact of seasons and different climates on the prevalence in the present meta-analysis, due to the limited data reported. Nonetheless, the heterogeneity after considering these confounding variables was still high. Other unknown and uninvestigated differences in study design and population might exist, but it is not uncommon for meta-analyses to have high heterogeneity. In addition to high heterogeneity, our study was also limited by the publication bias. This occurs when the results of studies influence the decision of the author or publisher. Therefore, we recommend developing a database of HIV patients infected with Cryptosporidium to estimate the overall prevalence of cryptosporidiosis and the geographical and time distribution of infection more accurately.
Conclusion
The prolonged and severe diarrhea caused by Cryptosporidium is associated with significant morbidity and mortality, especially in the HIV-infected population. This highlights the importance of preventive measures such as drinking safe water, using community-based or household water treatment systems, and education on hand hygiene after using toilets and before preparing food. Additionally, clinicians should consider early symptoms of cryptosporidiosis, such as diarrhea, in HIV patients, with the aim of initiating treatment early in the disease course. Also, patients with a CD4 count below 200 should receive prophylactic antiparasite treatment. If implemented correctly, these measures could lead to decreased morbidity, mortality, and transmission.
Conflict of interest
Authors declare there is no conflict of interest.
Funding
This study was supported by the Research Center for Evidence Based Medicine (RCEBM), Tabriz University of Medical Sciences, Tabriz, Iran.
Ehsan Ahmadpour and Hanie Safarpour contributed equally to the article.
References
- Adamu H, Petros B, Zhang G, Kassa H, Amer S, Ye J, Feng Y, Xiao L. 2014. Distribution and clinical manifestations of Cryptosporidium species and subtypes in HIV/AIDS patients in Ethiopia. PLOS Neglected Tropical Diseases, 8(4), e2831. [CrossRef] [PubMed] [Google Scholar]
- Adamu H, Wegayehu T, Petros B. 2013. High prevalence of diarrhoegenic intestinal parasite infections among non-ART HIV patients in Fitche Hospital. Ethiopia. PLoS One, 8(8), e72634. [CrossRef] [Google Scholar]
- Adhikari NA, Rai SK, Singh A, Dahal S, Ghimire G. 2006. Intestinal parasitic infections among HIV seropositive and high risk group subjects for HIV infection in Nepal. Nepal Medical College journal, 8(3), 166–170. [Google Scholar]
- Adjei A, Lartey M, Adiku T, Rodrigues O, Renner L, Sifah E, Mensah J, Akanmori B, Otchere J, Bentum B. 2003. Cryptosporidium oocysts in Ghanaian AIDS patients with diarrhoea. East African Medical Journal, 80(7), 369–372. [PubMed] [Google Scholar]
- Agholi M, Hatam GR, Motazedian MH. 2013. HIV/AIDS-associated opportunistic protozoal diarrhea. AIDS Research and Human Retroviruses, 29(1), 35–41. [CrossRef] [PubMed] [Google Scholar]
- Ahmed NH, Chowdhary A. 2013. Comparison of different methods of detection of enteric pathogenic protozoa. Indian Journal of Medical Microbiology, 31(2), 154–160. [PubMed] [Google Scholar]
- Ahmed NH, Chowdhary A. 2015. Pattern of co-infection by enteric pathogenic parasites among HIV sero-positive individuals in a Tertiary Care Hospital, Mumbai, India. Indian Journal of Sexually Transmitted Diseases and AIDS, 36(1), 40–47. [CrossRef] [PubMed] [Google Scholar]
- Akinbo FO, Okaka CE, Omoregie R. 2011. Prevalence of intestinal parasites in relation to CD4 counts and anaemia among HIV-infected patients in Benin City, Edo State. Nigeria. Tanzania Journal of Health Research, 13(1), 8–13. [Google Scholar]
- Akinbo FO, Okaka CE, Omoregie R, Adamu H, Xiao L. 2013. Unusual Enterocytozoon bieneusi genotypes and Cryptosporidium hominis subtypes in HIV-infected patients on highly active antiretroviral therapy. American Journal of Tropical Medicine and Hygiene, 89(1), 157–161. [CrossRef] [Google Scholar]
- Alemu A, Shiferaw Y, Getnet G, Yalew A, Addis Z. 2011. Opportunistic and other intestinal parasites among HIV/AIDS patients attending Gambi higher clinic in Bahir Dar city, North West Ethiopia. Asian Pacific Journal of Tropical Medicine, 4(8), 661–665. [CrossRef] [PubMed] [Google Scholar]
- Angal L, Mahmud R, Samin S, Yap NJ, Ngui R, Amir A, Ithoi I, Kamarulzaman A, Lim YA. 2015. Determining intestinal parasitic infections (IPIs) in inmates from Kajang Prison, Selangor, Malaysia for improved prison management. BMC Infectious Diseases, 15, 467. [CrossRef] [PubMed] [Google Scholar]
- Arenas-Pinto A, Certad G, Ferrara G, Castro J, Bello M, Nunez L. 2003. Association between parasitic intestinal infections and acute or chronic diarrhoea in HIV-infected patients in Caracas, Venezuela. International journal of STD & AIDS, 14(7), 487–492. [CrossRef] [PubMed] [Google Scholar]
- Asma I, Sim BL, Brent RD, Johari S, Yvonne Lim AL. 2015. Molecular epidemiology of Cryptosporidium in HIV/AIDS patients in Malaysia. Tropical Biomedicine, 32(2), 310–322. [PubMed] [Google Scholar]
- Assefa S, Erko B, Medhin G, Assefa Z, Shimelis T. 2009. Intestinal parasitic infections in relation to HIV/AIDS status, diarrhea and CD4 T-cell count. BMC Infectious Diseases, 9, 155. [CrossRef] [PubMed] [Google Scholar]
- Assis DC, Resende DV, Cabrine-Santos M, Correia D, Oliveira-Silva MB. 2013. Prevalence and genetic characterization of Cryptosporidium spp. and Cystoisospora belli in HIV-infected patients. Revista do Instituto de Medicina Tropical de Sao Paulo, 55(3), 149–154. [Google Scholar]
- Ayinmode AB, Zhang H, Dada-Adegbola HO, Xiao L. 2014. Cryptosporidium hominis subtypes and Enterocytozoon bieneusi genotypes in HIV-infected persons in Ibadan, Nigeria. Zoonoses and Public Health, 61(4), 297–303. [CrossRef] [PubMed] [Google Scholar]
- Bachur TP, Vale JM, Coelho IC, Queiroz TR, Chaves Cde S. 2008. Enteric parasitic infections in HIV/AIDS patients before and after the highly active antiretroviral therapy. Brazilian Journal of Infectious Diseases, 12(2), 115–122. [Google Scholar]
- Bartelt LA, Sevilleja JE, Barrett LJ, Warren CA, Guerrant RL, Bessong PO, Dillingham R, Samie A. 2013. High anti-Cryptosporidium parvum IgG seroprevalence in HIV-infected adults in Limpopo, South Africa. American Journal of Tropical Medicine and Hygiene, 89(3), 531–534. [CrossRef] [Google Scholar]
- Bern C, Kawai V, Vargas D, Rabke-Verani J, Williamson J, Chavez-Valdez R, Xiao L, Sulaiman I, Vivar A, Ticona E. 2005. The epidemiology of intestinal microsporidiosis in patients with HIV/AIDS in Lima, Peru. Journal of Infectious Diseases, 191(10), 1658–1664. [CrossRef] [Google Scholar]
- Blanco MA, Montoya A, Iborra A, Fuentes I. 2014. Identification of Cryptosporidium subtype isolates from HIV-seropositive patients in Equatorial Guinea. Transactions of the Royal Society of Tropical Medicine and Hygiene, 108(9), 594–596. [CrossRef] [PubMed] [Google Scholar]
- Boaitey YA, Nkrumah B, Idriss A, Tay SC. 2012. Gastrointestinal and urinary tract pathogenic infections among HIV seropositive patients at the Komfo Anokye Teaching Hospital in Ghana. BMC Research Notes, 5, 454. [CrossRef] [PubMed] [Google Scholar]
- Brink A-K, Mahe C, Watera C, Lugada E, Gilks C, Whitworth J, French N. 2002. Diarrhoea, CD4 counts and enteric infections in a community-based cohort of HIV-infected adults in Uganda. Journal of Infection, 45(2), 99–106. [CrossRef] [Google Scholar]
- Cama VA, Bern C, Sulaiman I, Gilman RH, Ticona E, Vivar A, Kawai V, Vargas D, Zhou L, Xiao L. 2003. Cryptosporidium species and genotypes in HIV-positive patients in Lima, Peru. Journal of Eukaryotic Microbiology, 50, 531–533. [CrossRef] [Google Scholar]
- Carcamo C, Hooton T, Wener MH, Weiss NS, Gilman R, Arevalo J, Carrasco J, Seas C, Caballero M, Holmes KK. 2005. Etiologies and manifestations of persistent diarrhea in adults with HIV-1 infection: a case-control study in Lima, Peru. Journal of Infectious Diseases, 191(1), 11–19. [CrossRef] [Google Scholar]
- Cardoso LV, Galisteu KJ, Schiesari Junior A, Chahla LA, Canille RM, Belloto MV, Franco C, Maia IL, Rossit AR, Machado RL. 2011. Enteric parasites in HIV-1/AIDS-infected patients from a Northwestern Sao Paulo reference unit in the highly active antiretroviral therapy era. Revista da Sociedade Brasileira de Medicina Tropical, 44(6), 665–669. [CrossRef] [PubMed] [Google Scholar]
- Certad G, Arenas-Pinto A, Pocaterra L, Ferrara G, Castro J, Bello A, Nunez L. 2005. Cryptosporidiosis in HIV-infected Venezuelan adults is strongly associated with acute or chronic diarrhea. American Journal of Tropical Medicine and Hygiene, 73(1), 54–57. [CrossRef] [Google Scholar]
- Chalmers RM, Campbell BM, Crouch N, Charlett A, Davies AP. 2011. Comparison of diagnostic sensitivity and specificity of seven Cryptosporidium assays used in the UK. Journal of Medical Microbiology, 60(Pt 11), 1598–1604. [CrossRef] [PubMed] [Google Scholar]
- Checkley W, White AC, Jaganath D, Arrowood MJ, Chalmers RM, Chen X-M, Fayer R, Griffiths JK, Guerrant RL, Hedstrom L, Huston CD, Kotloff KL, Kang G, Mead JR, Miller M, Petri WA, Priest JW, Roos DS, Striepen B, Thompson RCA, Ward HD, Van Voorhis WA, Xiao L, Zhu G, Houpt ER. 2015. A review of the global burden, novel diagnostics, therapeutics, and vaccine targets for cryptosporidium. Lancet Infectious Diseases, 15(1), 85–94. [Google Scholar]
- Chen X-M, Keithly JS, Paya CV, LaRusso NF. 2002. Cryptosporidiosis. New England Journal of Medicine, 346(22), 1723–1731. [CrossRef] [Google Scholar]
- Chhin S, Harwell JI, Bell JD, Rozycki G, Ellman T, Barnett JM, Ward H, Reinert SE, Pugatch D. 2006. Etiology of chronic diarrhea in antiretroviral-naive patients with HIV infection admitted to Norodom Sihanouk Hospital, Phnom Penh. Cambodia. Clinical Infectious Diseases, 43(7), 925–932. [CrossRef] [Google Scholar]
- Chokephaibulkit K, Wanachiwanawin D, Tosasuk K, Pavitpok J, Vanprapar N, Chearskul S. 2001. Intestinal parasitic infections among human immunodeficiency virus-infected and -uninfected children hospitalized with diarrhea in Bangkok, Thailand. Southeast Asian Journal of Tropical Medicine and Public Health, 32(4), 770–775. [Google Scholar]
- Colford JM Jr, Tager IB, Hirozawa AM, Lemp GF, Aragon T, Petersen C. 1996. Cryptosporidiosis among patients infected with human immunodeficiency virus: factors related to symptomatic infection and survival. American journal of epidemiology, 144(9), 807–816. [CrossRef] [PubMed] [Google Scholar]
- Cranendonk R, Kodde C, Chipeta D, Zijlstra E, Sluiters J. 2003. Cryptosporidium parvum and Isopora belli infections among patients with and without diarrhoea. East African medical journal, 80(8), 398–401. [PubMed] [Google Scholar]
- Daryani A, Sharif M, Meigouni M, Mahmoudi FB, Rafiei A, Gholami S, Khalilian A, Gohardehi S, Mirabi AM. 2009. Prevalence of intestinal parasites and profile of CD4+ counts in HIV+/AIDS people in north of Iran, 2007–2008. Pakistan Journal of Biological Sciences, 12(18), 1277–1281. [CrossRef] [Google Scholar]
- Dash M, Padhi S, Panda P, Parida B. 2013. Intestinal protozoans in adults with diarrhea. North American Journal of Medical Sciences, 5(12), 707–712. [CrossRef] [PubMed] [Google Scholar]
- de Oliveira-Silva MB, de Oliveira LR, Resende JC, Peghini BC, Ramirez LE, Lages-Silva E, Correia D. 2007. Seasonal profile and level of CD4+ lymphocytes in the occurrence of cryptosporidiosis and cystoisosporidiosis in HIV/AIDS patients in the Triangulo Mineiro region, Brazil. Revista da Sociedade Brasileira de Medicina Tropical, 40(5), 512–515. [CrossRef] [PubMed] [Google Scholar]
- Deeks J, Higgins J, Altman D, Green S. 2011. Cochrane handbook for systematic reviews of interventions version 5.1. 0 (updated March 2011). The Cochrane Collaboration. [Google Scholar]
- Dehkordy AB, Rafiei A, Alavi S, Latifi S. 2010. Prevalence of Cryptosporidium infection in immunocompromised patients, in South-west of Iran, 2009–10. Iranian Journal of Parasitology, 5(4), 42–47. [Google Scholar]
- Dillingham RA, Pinkerton R, Leger P, Severe P, Guerrant RL, Pape JW, Fitzgerald DW. 2009. High early mortality in patients with chronic acquired immunodeficiency syndrome diarrhea initiating antiretroviral therapy in Haiti: a case-control study. American Journal of Tropical Medicine and Hygiene, 80(6), 1060–1064. [CrossRef] [Google Scholar]
- Dwivedi KK, Prasad G, Saini S, Mahajan S, Lal S, Baveja UK. 2007. Enteric opportunistic parasites among HIV infected individuals: associated risk factors and immune status. Japanese Journal of Infectious Diseases, 60(2–3), 76–81. [PubMed] [Google Scholar]
- Erhabor O, Obunge O, Awah I. 2011. Cryptosporidiosis among HIV-infected persons in the Niger Delta of Nigeria. Nigerian Journal of Medicine, 20(3), 372–375. [Google Scholar]
- Eshetu T, Sibhatu G, Megiso M, Abere A, Baynes HW, Biadgo B, Zeleke AJ. 2017. Intestinal parasitosis and their associated factors among people living with HIV at University of Gondar Hospital, Northwest-Ethiopia. Ethiopian Journal of Health Sciences, 27(4), 411–420. [CrossRef] [PubMed] [Google Scholar]
- Feng Y, Ryan UM, Xiao L. 2018. Genetic diversity and population structure of Cryptosporidium. Trends in Parasitology, 34(11), 997–1011. [CrossRef] [PubMed] [Google Scholar]
- Framm SR, Soave R. 1997. Agents of diarrhea. Medical Clinics of North America, 81(2), 427–447. [CrossRef] [Google Scholar]
- Fregonesi BM, Suzuki MN, Machado CS, Tonani KA, Fernandes AP, Monroe AA, Cervi MC, Segura-Munoz S. 2015. Emergent and re-emergent parasites in HIV-infected children: immunological and socio-environmental conditions that are involved in the transmission of Giardia spp. and Cryptosporidium spp. Revista da Sociedade Brasileira de Medicina Tropical, 48(6), 753–758. [CrossRef] [PubMed] [Google Scholar]
- Gassama A, Sow PS, Fall F, Camara P, Philippe H, Guèye-N’Diaye A, Seng R, Samb B, M’Boup S, Germani Y. 2001. Ordinary and opportunistic enteropathogens associated with diarrhea in Senegalese adults in relation to human immunodeficiency virus serostatus. International Journal of Infectious Diseases, 5(4), 192–198. [CrossRef] [Google Scholar]
- Gautam H, Bhalla P, Saini S, Uppal B, Kaur R, Baveja CP, Dewan R. 2009. Epidemiology of opportunistic infections and its correlation with CD4 T-lymphocyte counts and plasma viral load among HIV-positive patients at a tertiary care hospital in India. Journal of the International Association of Physicians in AIDS Care, 8(6), 333–337. [CrossRef] [PubMed] [Google Scholar]
- Gedle D, Kumera G, Eshete T, Ketema K, Adugna H, Feyera F. 2017. Intestinal parasitic infections and its association with undernutrition and CD4 T cell levels among HIV/AIDS patients on HAART in Butajira, Ethiopia. Journal of Health, Population and Nutrition, 36(1), 15. [CrossRef] [Google Scholar]
- Getaneh A, Medhin G, Shimelis T. 2010. Cryptosporidium and Strongyloides stercoralis infections among people with and without HIV infection and efficiency of diagnostic methods for Strongyloides in Yirgalem Hospital, southern Ethiopia. BMC Research Notes, 3, 90. [CrossRef] [PubMed] [Google Scholar]
- Ghafari R, Rafiei A, Tavalla M, Moradi Choghakabodi P, Nashibi R, Rafiei R. 2018. Prevalence of Cryptosporidium species isolated from HIV/AIDS patients in southwest of Iran. Comparative Immunology, Microbiology & Infectious Diseases, 56, 39–44. [CrossRef] [Google Scholar]
- Gholami R, Gholami S, Emadi-Kouchak H, Abdollahi A, Shahriari M. 2016. Clinical Characteristic of the HIV/AIDS patients with cryptosporidiosis referring to Behavioral Diseases Consultation Center, Imam Khomeini Hospital, Tehran in 2013. Iranian Journal of Pathology, 11(1), 27–34. [PubMed] [Google Scholar]
- Girma M, Teshome W, Petros B, Endeshaw T. 2014. Cryptosporidiosis and Isosporiasis among HIV-positive individuals in south Ethiopia: a cross sectional study. BMC Infectious Diseases, 14, 100. [CrossRef] [PubMed] [Google Scholar]
- Gualberto FA, Heller L. 2006. Endemic Cryptosporidium infection and drinking water source: a systematic review and meta-analyses. Water Science and Technology, 54(3), 231–238. [CrossRef] [Google Scholar]
- Guk SM, Seo M, Park YK, Oh MD, Choe KW, Kim JL, Choi MH, Hong ST, Chai JY. 2005. Parasitic infections in HIV-infected patients who visited Seoul National University Hospital during the period 1995–2003. Korean Journal of Parasitology, 43(1), 1–5. [CrossRef] [Google Scholar]
- Gupta K, Bala M, Deb M, Muralidhar S, Sharma DK. 2013. Prevalence of intestinal parasitic infections in HIV-infected individuals and their relationship with immune status. Indian Journal of Medical Microbiology, 31(2), 161–165. [PubMed] [Google Scholar]
- Gupta S, Narang S, Nunavath V, Singh S. 2008. Chronic diarrhoea in HIV patients: prevalence of coccidian parasites. Indian Journal of Medical Microbiology, 26(2), 172–175. [CrossRef] [PubMed] [Google Scholar]
- Hailu AW, G/Selassie S, Merid Y, Gebru AA, Ayene YY, Asefa MK. 2015. The case control studies of HIV and intestinal parasitic infections rate in active pulmonary tuberculosis patients in Woldia General Hospital and Health Center in North Wollo, Amhara Region, Ethiopia. International Journal of Pharma Sciences, 5(3), 1092–1099. [PubMed] [Google Scholar]
- Houpt ER, Bushen OY, Sam NE, Kohli A, Asgharpour A, Ng CT, Calfee DP, Guerrant RL, Maro V, Ole-Nguyaine S, Shao JF. 2005. Short report: asymptomatic Cryptosporidium hominis infection among human immunodeficiency virus-infected patients in Tanzania. American Journal of Tropical Medicine and Hygiene, 73(3), 520–522. [CrossRef] [Google Scholar]
- Hung CC, Tsaihong JC, Lee YT, Deng HY, Hsiao WH, Chang SY, Chang SC, Su KE. 2007. Prevalence of intestinal infection due to Cryptosporidium species among Taiwanese patients with human immunodeficiency virus infection. Journal of the Formosan Medical Association, 106(1), 31–35. [CrossRef] [Google Scholar]
- Hunter PR, Nichols G. 2002. Epidemiology and clinical features of Cryptosporidium infection in immunocompromised patients. Clinical Microbiology Reviews, 15(1), 145–154. [CrossRef] [PubMed] [Google Scholar]
- Idris NS, Dwipoerwantoro PG, Kurniawan A, Said M. 2010. Intestinal parasitic infection of immunocompromised children with diarrhoea: clinical profile and therapeutic response. Journal of Infection in Developing Countries, 4(5), 309–317. [CrossRef] [PubMed] [Google Scholar]
- Inungu J, Morse A, Gordon C. 2000. Risk factors, seasonality, and trends of cryptosporidiosis among patients infected with human immunodeficiency virus. American Journal of Tropical Medicine and Hygiene, 62(3), 384–387. [CrossRef] [Google Scholar]
- Iqbal A, Lim YA, Surin J, Sim BL. 2012. High diversity of Cryptosporidium subgenotypes identified in Malaysian HIV/AIDS individuals targeting gp60 gene. PLoS One, 7(2), e31139. [CrossRef] [PubMed] [Google Scholar]
- Irisarri-Gutierrez MJ, Mingo MH, de Lucio A, Gil H, Morales L, Segui R, Nacarapa E, Munoz-Antoli C, Bornay-Llinares FJ, Esteban JG, Carmena D. 2017. Association between enteric protozoan parasites and gastrointestinal illness among HIV- and tuberculosis-infected individuals in the Chowke district, southern Mozambique. Acta Tropica, 170, 197–203. [CrossRef] [PubMed] [Google Scholar]
- Izadi M, Jonaidi-Jafari N, Saburi A, Eyni H, Rezaiemanesh MR, Ranjbar R. 2012. Prevalence, molecular characteristics and risk factors for cryptosporidiosis among Iranian immunocompromised patients. Microbiology and Immunology, 56(12), 836–842. [CrossRef] [PubMed] [Google Scholar]
- Jagai JS, Castronovo DA, Monchak J, Naumova EN. 2009. Seasonality of cryptosporidiosis: A meta-analysis approach. Environmental Research, 109(4), 465–478. [CrossRef] [PubMed] [Google Scholar]
- Janagond AB, Sasikala G, Agatha D, Ravinder T, Thenmozhivalli PR. 2013. Enteric parasitic infections in relation to diarrhoea in HIV infected individuals with CD4 T Cell Counts <1000 Cells/mul in Chennai, India. Journal of Clinical and Diagnostic Research, 7(10), 2160–2162. [Google Scholar]
- Jayalakshmi J, Appalaraju B, Mahadevan K. 2008. Evaluation of an enzyme-linked immunoassay for the detection of Cryptosporidium antigen in fecal specimens of HIV/AIDS patients. Indian Journal of Pathology and Microbiology, 51(1), 137–138. [CrossRef] [Google Scholar]
- Jha AK, Uppal B, Chadha S, Bhalla P, Ghosh R, Aggarwal P, Dewan R. 2012. Clinical and microbiological profile of HIV/AIDS cases with diarrhea in North India. Journal of Pathogens, 2012, 971958. [PubMed] [Google Scholar]
- Joshi M, Chowdhary A, Dalai P, Maniar J. 2002. Parasitic diarrhoea in patients with AIDS. National Medical Journal of India, 15(2), 72–74. [Google Scholar]
- Rashmi KS, Kumar KLR. 2013. Intestinal cryptosporidiosis and the profile of the CD4 Counts in a cohort of HIV infected patients. Journal of Clinical and Diagnostic Research, 7(6), 1016–1020. [Google Scholar]
- Kange’the E, McDermott B, Grace D, Mbae C, Mulinge E, Monda J, Nyongesa C, Ambia J, Njehu A. 2012. Prevalence of cryptosporidiosis in dairy cattle, cattle-keeping families, their non-cattle-keeping neighbours and HIV-positive individuals in Dagoretti Division, Nairobi, Kenya. Tropical Animal Health and Production, 44(Suppl 1), S11–S16. [CrossRef] [PubMed] [Google Scholar]
- Kaniyarakkal V, Mundangalam N, Moorkoth AP, Mathew S. 2016. Intestinal parasite profile in the stool of HIV positive patients in relation to immune status and comparison of various diagnostic techniques with special reference to Cryptosporidium at a tertiary care hospital in South India. Advances in Medical Sciences, 2016, 3564359. [Google Scholar]
- Kashyap B, Sinha S, Das S, Rustagi N, Jhamb R. 2010. Efficiency of diagnostic methods for correlation between prevalence of enteric protozoan parasites and HIV/AIDS status–an experience of a tertiary care hospital in East Delhi. Journal of Parasitic Diseases, 34(2), 63–67. [CrossRef] [Google Scholar]
- Kaushik K, Khurana S, Wanchu A, Malla N. 2008. Evaluation of staining techniques, antigen detection and nested PCR for the diagnosis of cryptosporidiosis in HIV seropositive and seronegative patients. Acta Tropica, 107(1), 1–7. [CrossRef] [PubMed] [Google Scholar]
- Khalil S, Mirdha BR, Sinha S, Panda A, Singh Y, Joseph A, Deb M. 2015. Intestinal parasitosis in relation to anti-retroviral therapy, CD4(+) T-cell count and diarrhea in HIV patients. Korean Journal of Parasitology, 53(6), 705–712. [CrossRef] [Google Scholar]
- Khurana S, Sharma P, Sharma A, Malla N. 2012. Evaluation of Ziehl-Neelsen staining, auramine phenol staining, antigen detection enzyme linked immunosorbent assay and polymerase chain reaction, for the diagnosis of intestinal cryptosporidiosis. Tropical Parasitology, 2(1), 20–23. [CrossRef] [PubMed] [Google Scholar]
- Kiros H, Nibret E, Munshea A, Kerisew B, Adal M. 2015. Prevalence of intestinal protozoan infections among individuals living with HIV/AIDS at Felegehiwot Referral Hospital, Bahir Dar, Ethiopia. International Journal of Infectious Diseases, 35, 80–86. [CrossRef] [Google Scholar]
- Kucerova Z, Sokolova OI, Demyanov AV, Kvac M, Sak B, Kvetonova D, Secor WE. 2011. Microsporidiosis and cryptosporidiosis in HIV/AIDS Patients in St. Petersburg, Russia: Serological identification of microsporidia and Cryptosporidium parvum in sera samples from HIV/AIDS patients. AIDS Research and Human Retroviruses, 27(1), 13–15. [CrossRef] [PubMed] [Google Scholar]
- Kulkarni SV, Kairon R, Sane SS, Padmawar PS, Kale VA, Thakar MR, Mehendale SM, Risbud AR. 2009. Opportunistic parasitic infections in HIV/AIDS patients presenting with diarrhoea by the level of immunesuppression. Indian Journal of Medical Research, 130(1), 63–66. [Google Scholar]
- Kumar SS, Ananthan S, Lakshmi P. 2002. Intestinal parasitic infection in HIV infected patients with diarrhoea in Chennai. Indian Journal of Medical Microbiology, 20(2), 88. [PubMed] [Google Scholar]
- Kurniawan A, Karyadi T, Dwintasari SW, Sari IP, Yunihastuti E, Djauzi S, Smith HV. 2009. Intestinal parasitic infections in HIV/AIDS patients presenting with diarrhoea in Jakarta, Indonesia. Transactions of the Royal Society of Tropical Medicine and Hygiene, 103(9), 892–898. [CrossRef] [PubMed] [Google Scholar]
- Kwakye-Nuako G, Boampong JN, Dong MK, Obiri-Yeboah D, Opoku YK, Amoako-Sakyi D, Asare KK. 2016. Modulation of cyptosporidiosis by CD4 levels in chronic diarrhoea HIV/AIDS individuals visiting Tarkwa Municipal hospital, Ghana. Asian Pacific Journal of Tropical Disease, 6(10), 770–775. [Google Scholar]
- Leav BA, Mackay MR, Anyanwu A, O’Connor RM, Cevallos AM, Kindra G, Rollins NC, Bennish ML, Nelson RG, Ward HD. 2002. Analysis of sequence diversity at the highly polymorphic Cpgp40/15 locus among Cryptosporidium isolates from human immunodeficiency virus-infected children in South Africa. Infection and Immunity, 70(7), 3881–3890. [CrossRef] [PubMed] [Google Scholar]
- Lebbad M, Norrgren H, Nauclér A, Dias F, Andersson S, Linder E. 2001. Intestinal parasites in HIV-2 associated AIDS cases with chronic diarrhoea in Guinea-Bissau. Acta Tropica, 80(1), 45–49. [CrossRef] [PubMed] [Google Scholar]
- Lehman LG, Kangam L, Mbenoun ML, Zemo Nguepi E, Essomba N, Tonga C, Bilong Bilong CF. 2013. Intestinal parasitic and candida infection associated with HIV infection in Cameroon. Journal of Infection in Developing Countries, 7(2), 137–143. [CrossRef] [PubMed] [Google Scholar]
- Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, Clarke M, Devereaux PJ, Kleijnen J, Moher D. 2009. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. PLOS Medicine, 6(7), e1000100. [Google Scholar]
- Lim YA, Iqbal A, Surin J, Sim BL, Jex AR, Nolan MJ, Smith HV, Gasser RB. 2011. First genetic classification of Cryptosporidium and Giardia from HIV/AIDS patients in Malaysia. Infection, Genetics and Evolution, 11(5), 968–974. [CrossRef] [Google Scholar]
- Lim YA, Rohela M, Sim BL, Jamaiah I, Nurbayah M. 2005. Prevalence of cryptosporidiosis in HIV-infected patients in Kajang Hospital, Selangor. Southeast Asian Journal of Tropical Medicine and Public Health, 36(Suppl 4), 30–33. [Google Scholar]
- Lule JR, Mermin J, Awor A, Hughes P, Kigozi A, Wafula W, Nakanjako D, Kaharuza F, Downing R, Quick R. 2009. Aetiology of diarrhoea among persons with HIV and their family members in rural Uganda: a community-based study. East African Medical Journal, 86(9), 422–429. [PubMed] [Google Scholar]
- Marques FR, Cardoso LV, Cavasini CE, Almeida MC, Bassi NA, Almeida MT, Rossit AR, Machado RL. 2005. Performance of an immunoenzymatic assay for Cryptosporidium diagnosis of fecal samples. Brazilian Journal of Infectious Diseases, 9(1), 3–5. [Google Scholar]
- Masarat S, Ahmad F, Chisti M, Hamid S, Sofi BA. 2012. Prevalence of Cryptosporidium species among HIV positive asymptomatic and symptomatic immigrant population in Kashmir, India. Iranian Journal of Microbiology, 4(1), 35–39. [PubMed] [Google Scholar]
- Mathur MK, Verma AK, Makwana GE, Sinha M. 2013. Study of opportunistic intestinal parasitic infections in human immunodeficiency virus/acquired immunodeficiency syndrome patients. Journal of Global Infectious Diseases, 5(4), 164–167. [CrossRef] [PubMed] [Google Scholar]
- Mehta KD, Vacchani A, Mistry MM, Kavathia GU, Goswami YS. 2013. To study the prevalence of various enteric parasitic infections among HIV infected individuals in the P.D.U. Medical College and Hospital, Rajkot, Gujarat, India. Journal of Clinical and Diagnostic Research, 7(1), 58–60. [Google Scholar]
- Mengist HM, Taye B, Tsegaye A. 2015. Intestinal parasitosis in relation to CD4+T cells levels and anemia among HAART initiated and HAART naive pediatric HIV patients in a model ART center in Addis Ababa, Ethiopia. PLoS One, 10(2), e0117715. [CrossRef] [PubMed] [Google Scholar]
- Missaye A, Dagnew M, Alemu A, Alemu A. 2013. Prevalence of intestinal parasites and associated risk factors among HIV/AIDS patients with pre-ART and on-ART attending dessie hospital ART clinic, Northeast Ethiopia. AIDS Research and Therapy, 10(1), 7. [CrossRef] [PubMed] [Google Scholar]
- Mitra S, Mukherjee A, Khanra D, Bhowmik A, Roy K, Talukdar A. 2016. Enteric parasitic infection among antiretroviral therapy naive HIV-seropositive people: infection begets infection-experience from Eastern India. Journal of Global Infectious Diseases, 8(2), 82–86. [CrossRef] [PubMed] [Google Scholar]
- Moss PJ, Read RC, Kudesia G, McKendrick MW. 1995. Prolonged cryptosporidiosis during primary HIV infection. Journal of Infection, 30(1), 51–53. [CrossRef] [Google Scholar]
- Mohandas K, Sehgal R, Sud A, Malla N. 2002. Prevalence of intestinal parasitic pathogens in HIV-seropositive individuals in Northern India. Japanese journal of infectious diseases, 55(3), 83–84. [PubMed] [Google Scholar]
- Mohanty I, Panda P, Sahu S, Dash M, Narasimham MV, Padhi S, Parida B. 2013. Prevalence of isosporiasis in relation to CD4 cell counts among HIV-infected patients with diarrhea in Odisha, India. Advanced Biomedical Research, 2, 61. [CrossRef] [PubMed] [Google Scholar]
- Monkemuller KE, Wilcox CM. 2000. Investigation of diarrhea in AIDS. Canadian Journal of Gastroenterology and Hepatology, 14(11), 933–940. [Google Scholar]
- Navarro-i-Martinez L, da Silva AJ, Botero Garces JH, Montoya Palacio MN, del Aguila C, Bornay-Llinares FJ. 2006. Cryptosporidiosis in HIV-positive patients from Medellin, Colombia. Journal of Eukaryotic Microbiology, 53(Suppl 1), S37–S39. [CrossRef] [Google Scholar]
- Navin TR, Juranek DD. 1984. Cryptosporidiosis: clinical, epidemiologic, and parasitologic review. Reviews of Infectious Diseases, 6(3), 313–327. [CrossRef] [PubMed] [Google Scholar]
- Navin TR, Weber R, Vugia DJ, Rimland D, Roberts JM, Addiss DG, Visvesvara GS, Wahlquist SP, Hogan SE, Gallagher LE, Juranek DD, Schwartz DA, Wilcox CM, Stewart JM, Thompson SE 3rd, Bryan RT. 1999. Declining CD4+ T-lymphocyte counts are associated with increased risk of enteric parasitosis and chronic diarrhea: results of a 3-year longitudinal study. Journal of Acquired Immune Deficiency Syndromes and Human Retrovirology, 20(2), 154–159. [CrossRef] [Google Scholar]
- Netor Velasquez J, Marta E, Alicia di Risio C, Etchart C, Gancedo E, Victor Chertcoff A, Bruno Malandrini J, German Astudillo O, Carnevale S. 2012. Molecular identification of protozoa causing AIDS-associated cholangiopathy in Buenos Aires, Argentina. Acta Gastroenterologica Latinoamericana, 42(4), 301–308. [PubMed] [Google Scholar]
- Nsagha DS, Njunda AL, Assob NJC, Ayima CW, Tanue EA, Kibu OD, Kwenti TE. 2016. Intestinal parasitic infections in relation to CD4(+) T cell counts and diarrhea in HIV/AIDS patients with or without antiretroviral therapy in Cameroon. BMC Infectious Diseases, 16, 9. [CrossRef] [PubMed] [Google Scholar]
- Nuchjangreed C, Boonrod K, Ongerth J, Karanis P. 2008. Prevalence and molecular characterization of human and bovine Cryptosporidium isolates in Thailand. Parasitology Research, 103(6), 1347–1353. [CrossRef] [PubMed] [Google Scholar]
- Obateru OA, Bojuwoye BJ, Olokoba AB, Fadeyi A, Fowotade A, Olokoba LB. 2017. Prevalence of intestinal parasites in newly diagnosed HIV/AIDS patients in Ilorin, Nigeria. Alexandria Journal of Medicine, 53(2), 111–116. [CrossRef] [Google Scholar]
- Oguntibeju OO. 2006. Prevalence of intestinal parasites in HIV-positive/AIDS patients. Malaysian Journal of Medical Sciences, 13(1), 68–73. [Google Scholar]
- Ojuromi OT, Duan L, Izquierdo F, Fenoy SM, Oyibo WA, Del Aguila C, Ashafa AO, Feng Y, Xiao L. 2016. Genotypes of Cryptosporidium spp. and Enterocytozoon bieneusi in human immunodeficiency virus-infected patients in Lagos, Nigeria. Journal of Eukaryotic Microbiology, 63(4), 414–418. [CrossRef] [Google Scholar]
- Ojuromi OT, Izquierdo F, Fenoy S, Fagbenro-Beyioku A, Oyibo W, Akanmu A, Odunukwe N, Henriques-Gil N, del Aguila C. 2012. Identification and characterization of microsporidia from fecal samples of HIV-positive patients from Lagos. Nigeria. PLoS One, 7(4), e35239. [CrossRef] [Google Scholar]
- Ojurongbe O, Raji OA, Akindele AA, Kareem MI, Adefioye OA, Adeyeba AO. 2011. Cryptosporidium and other enteric parasitic infections in HIV-seropositive individuals with and without diarrhoea in Osogbo, Nigeria. British Journal of Biomedical Science, 68(2), 75–78. [CrossRef] [PubMed] [Google Scholar]
- Omoruyi BE, Nwodo UU, Udem CS, Okonkwo FO. 2014. Comparative diagnostic techniques for Cryptosporidium infection. Molecules, 19(2), 2674–2683. [CrossRef] [PubMed] [Google Scholar]
- Oyedeji OA, Adejuyigbe E, Oninla SO, Akindele AA, Adedokun SA, Agelebe E. 2015. Intestinal parasitoses in HIV infected children in a Nigerian tertiary hospital. Journal of Clinical and Diagnostic Research, 9(11), Sc01-5. [Google Scholar]
- Paboriboune P, Phoumindr N, Borel E, Sourinphoumy K, Phaxayaseng S, Luangkhot E, Sengphilom B, Vansilalom Y, Odermatt P, Delaporte E, Etard JF, Rabodonirina M. 2014. Intestinal parasitic infections in HIV-infected patients, Lao People’s Democratic Republic. PLoS One, 9(3), e91452. [CrossRef] [PubMed] [Google Scholar]
- Pantenburg B, Dann SM, Wang H-C, Robinson P, Castellanos-Gonzalez A, Lewis DE, White AC. 2008. Intestinal immune response to human Cryptosporidium sp. infection. Infection and Immunity, 76(1), 23–29. [CrossRef] [PubMed] [Google Scholar]
- Parghi E, Dash L, Shastri J. 2014. Evaluation of different modifications of acid-fast staining techniques and stool enzyme-linked immunosorbent assay in detecting fecal Cryptosporidium in diarrheic HIV seropositive and seronegative patients. Tropical Parasitology, 4(2), 99–104. [CrossRef] [PubMed] [Google Scholar]
- Patel SD, Kinariwala DM, Javadekar TB. 2011. Clinico-microbiological study of opportunistic infection in HIV seropositive patients. Indian Journal of Sexually Transmitted Diseases and AIDS, 32(2), 90–93. [CrossRef] [PubMed] [Google Scholar]
- Pavie J, Menotti J, Porcher R, Donay JL, Gallien S, Sarfati C, Derouin F, Molina JM. 2012. Prevalence of opportunistic intestinal parasitic infections among HIV-infected patients with low CD4 cells counts in France in the combination antiretroviral therapy era. International Journal of Infectious Diseases, 16(9), e677–e679. [CrossRef] [Google Scholar]
- Pavlinac PB, John-Stewart GC, Naulikha JM, Onchiri FM, Denno DM, Odundo EA, Singa BO, Richardson BA, Walson JL. 2014. High-risk enteric pathogens associated with HIV infection and HIV exposure in Kenyan children with acute diarrhoea. AIDS, 28(15), 2287–2296. [CrossRef] [PubMed] [Google Scholar]
- Petrincova A, Valencakova A, Luptakova L, Ondriska F, Kalinova J, Halanova M, Danisova O, Jarcuska P. 2015. Molecular characterization and first report of Cryptosporidium genotypes in human population in the Slovak Republic. Electrophoresis, 36(23), 2925–2930. [CrossRef] [PubMed] [Google Scholar]
- Pinlaor S, Mootsikapun P, Pinlaor P, Pipitgool V, Tuangnadee R. 2005. Detection of opportunistic and non-opportunistic intestinal parasites and liver flukes in HIV-positive and HIV-negative subjects. Southeast Asian Journal of Tropical Medicine and Public Health, 36(4), 841–845. [Google Scholar]
- Raccurt CP, Fouche B, Agnamey P, Menotti J, Chouaki T, Totet A, Pape JW. 2008. Presence of Enterocytozoon bieneusi associated with intestinal coccidia in patients with chronic diarrhea visiting an HIV center in Haiti. American Journal of Tropical Medicine and Hygiene, 79(4), 579–580. [CrossRef] [Google Scholar]
- Ramakrishnan K, Shenbagarathai R, Uma A, Kavitha K, Rajendran R, Thirumalaikolundusubramanian P. 2007. Prevalence of intestinal parasitic infestation in HIV/AIDS patients with diarrhea in Madurai City, South India. Japanese Journal of Infectious Diseases, 60(4), 209–210. [PubMed] [Google Scholar]
- Ribeiro PC, Pile E, Queiroz MMdC, Norberg AN, Tenório JRdO. 2004. Cryptosporidiosis occurrence in HIV+ patients attended in a hospital, Brazil. Revista de Saúde Pública, 38(3), 469–470. [CrossRef] [Google Scholar]
- Roka M, Goni P, Rubio E, Clavel A. 2012. Prevalence of intestinal parasites in HIV-positive patients on the island of Bioko, Equatorial Guinea: its relation to sanitary conditions and socioeconomic factors. Science of the Total Environment, 432, 404–411. [CrossRef] [Google Scholar]
- Rossit AR, de Almeida MT, Nogueira CA, da Costa Oliveira JG, Barbosa DM, Moscardini AC, Mascarenhas JD, Gabbay YB, Marques FR, Cardoso LV, Cavasini CE, Machado RL. 2007. Bacterial, yeast, parasitic, and viral enteropathogens in HIV-infected children from Sao Paulo State, Southeastern Brazil. Diagnostic Microbiology and Infectious Disease, 57(1), 59–66. [CrossRef] [PubMed] [Google Scholar]
- Sadraei J, Rizvi MA, Baveja UK. 2005. Diarrhea, CD4+ cell counts and opportunistic protozoa in Indian HIV-infected patients. Parasitology Research, 97(4), 270–273. [CrossRef] [PubMed] [Google Scholar]
- Saksirisampant W, Eampokalap B, Rattanasrithong M, Likanonsakul S, Wiwanitkit V, Nasingkarn A, Denmasae N. 2002. A prevalence of Cryptosporidium infections among Thai HIV-infected patients. Journal of the Medical Association of Thailand = Chotmaihet thangphaet, 85, S424–S428. [PubMed] [Google Scholar]
- Saksirisampant W, Prownebon J, Saksirisampant P, Mungthin M, Siripatanapipong S, Leelayoova S. 2009. Intestinal parasitic infections: Prevalences in HIV/AIDS patients in a Thai AIDS-care centre. Annals of Tropical Medicine & Parasitology, 103(7), 573–581. [CrossRef] [Google Scholar]
- Salehi Sangani G, Mirjalali H, Farnia S, Rezaeian M. 2016. Prevalence of intestinal coccidial infections among different groups of immunocompromised patients. Iranian Journal of Parasitology, 11(3), 332–338. [PubMed] [Google Scholar]
- Samie A, Makuwa S, Mtshali S, Potgieter N, Thekisoe O, Mbati P, Bessong PO. 2014. Parasitic infection among HIV/AIDS patients at Bela-Bela clinic, Limpopo province, South Africa with special reference to Cryptosporidium. Southeast Asian Journal of Tropical Medicine and Public Health, 45(4), 783–795. [Google Scholar]
- Sanchez JM. 2016. An exercise in sampling: The effect of sample size and number of samples on sampling error. World Journal of Chemical Education, 4(2), 45–48. [Google Scholar]
- Santos RB, Fonseca LE Jr, Santana AT, Silva CA, Guedes JC. 2011. Clinical, endoscopic and histopathological profiles of parasitic duodenitis cases diagnosed by upper digestive endoscopy. Arquivos de Gastroenterologia, 48(4), 225–230. [CrossRef] [PubMed] [Google Scholar]
- Sarfati C, Bourgeois A, Menotti J, Liegeois F, Moyou-Somo R, Delaporte E, Derouin F, Ngole EM, Molina JM. 2006. Prevalence of intestinal parasites including microsporidia in human immunodeficiency virus-infected adults in Cameroon: a cross-sectional study. American Journal of Tropical Medicine and Hygiene, 74(1), 162–164. [CrossRef] [Google Scholar]
- Shah S, Kongre V, Kumar V, Bharadwaj R. 2016. A study of parasitic and bacterial pathogens associated with diarrhea in HIV-positive patients. Cureus, 8(9), e807. [PubMed] [Google Scholar]
- Sharma P, Sharma A, Sehgal R, Malla N, Khurana S. 2013. Genetic diversity of Cryptosporidium isolates from patients in North India. International Journal of Infectious Diseases, 17(8), e601–e605. [CrossRef] [Google Scholar]
- Shenoy S, Baliga S, Kurnvilla T, Prashanth H, Dominic RS. 2003. Opportunistic intestinal parasitic infections in human immunodeficiency virus infected patients in Mangalore. South India. Tropical Doctor, 33(4), 250. [CrossRef] [Google Scholar]
- Shimelis T, Tadesse E. 2014. Performance evaluation of point-of-care test for detection of Cryptosporidium stool antigen in children and HIV infected adults. Parasites & Vectors, 7, 227. [CrossRef] [PubMed] [Google Scholar]
- Shimelis T, Tassachew Y, Lambiyo T. 2016. Cryptosporidium and other intestinal parasitic infections among HIV patients in southern Ethiopia: significance of improved HIV-related care. Parasites & Vectors, 9(1), 270. [CrossRef] [PubMed] [Google Scholar]
- Silva CV, Ferreira MS, Borges AS, Costa-Cruz JM. 2005. Intestinal parasitic infections in HIV/AIDS patients: experience at a teaching hospital in central Brazil. Scandinavian Journal of Infectious Diseases, 37(3), 211–215. [CrossRef] [PubMed] [Google Scholar]
- Silva CV, Ferreira MS, Gonçalves-Pires MdRd, Costa-Cruz JM. 2003. Detection of Cryptosporidium-specific coproantigen in human immunodeficiency virus/acquired immunodeficiency syndrome patients by using a commercially available immunoenzymatic assay. Memórias do Instituto Oswaldo Cruz, 98(8), 1097–1099. [CrossRef] [Google Scholar]
- Singh A, Bairy I, Shivananda P. 2003. Spectrum of opportunistic infections in AIDS cases. Indian Journal of Medical Sciences, 57(1), 16–21. [PubMed] [Google Scholar]
- Srisuphanunt M, Saksirisampant W, Karanis P. 2011. Prevalence and genotyping of Cryptosporidium isolated from HIV/AIDS patients in urban areas of Thailand. Annals of Tropical Medicine & Parasitology, 105(6), 463–468. [CrossRef] [PubMed] [Google Scholar]
- Stark D, Fotedar R, van Hal S, Beebe N, Marriott D, Ellis JT, Harkness J. 2007. Prevalence of enteric protozoa in human immunodeficiency virus (HIV)-positive and HIV-negative men who have sex with men from Sydney, Australia. American Journal of Tropical Medicine and Hygiene, 76(3), 549–552. [CrossRef] [Google Scholar]
- Stensvold CR, Nielsen SD, Badsberg JH, Engberg J, Friis-Moller N, Nielsen SS, Nielsen HV, Friis-Moller A. 2011. The prevalence and clinical significance of intestinal parasites in HIV-infected patients in Denmark. Scandinavian Journal of Infectious Diseases, 43(2), 129–135. [CrossRef] [PubMed] [Google Scholar]
- Swathirajan CR, Vignesh R, Pradeep A, Solomon SS, Solomon S, Balakrishnan P. 2017. Occurrence of enteric parasitic infections among HIV-infected individuals and its relation to CD4 T-cell counts with a special emphasis on coccidian parasites at a tertiary care centre in South India. Indian Journal of Medical Microbiology, 35(1), 37–40. [CrossRef] [PubMed] [Google Scholar]
- Tadesse A, Kassu A. 2005. Intestinal parasite isolates in AIDS patients with chronic diarrhea in Gondar Teaching Hospital, North west Ethiopia. Ethiopian Medical Journal, 43(2), 93–96. [PubMed] [Google Scholar]
- Taherkhani H, Fallah M, Jadidian K, Vaziri S. 2007. A study on the prevalence of Cryptosporidium in HIV positive patients. Journal of Research in Health Sciences, 7(2), 20–24. [PubMed] [Google Scholar]
- Taye B, Desta K, Ejigu S, Dori GU. 2014. The magnitude and risk factors of intestinal parasitic infection in relation to Human Immunodeficiency Virus infection and immune status, at ALERT Hospital, Addis Ababa, Ethiopia. Parasitology International, 63(3), 550–556. [CrossRef] [PubMed] [Google Scholar]
- Teklemariam Z, Abate D, Mitiku H, Dessie Y. 2013. Prevalence of intestinal parasitic infection among HIV positive persons who are naive and on antiretroviral treatment in Hiwot Fana specialized University Hospital, Eastern Ethiopia. International Scholarly Research Notices, 2013, 324329. [Google Scholar]
- Tellevik MG, Moyo SJ, Blomberg B, Hjollo T, Maselle SY, Langeland N, Hanevik K. 2015. Prevalence of Cryptosporidium parvum/hominis, Entamoeba histolytica and Giardia lamblia among young children with and without diarrhea in Dar es Salaam, Tanzania. PLOS Neglected Tropical Diseases, 9(10), e0004125. [CrossRef] [PubMed] [Google Scholar]
- Tian LG, Chen JX, Wang TP, Cheng GJ, Steinmann P, Wang FF, Cai YC, Yin XM, Guo J, Zhou L, Zhou XN. 2012. Co-infection of HIV and intestinal parasites in rural area of China. Parasites & Vectors, 5, 36. [CrossRef] [PubMed] [Google Scholar]
- Tian LG, Wang TP, Lv S, Wang FF, Guo J, Yin XM, Cai YC, Dickey MK, Steinmann P, Chen JX. 2013. HIV and intestinal parasite co-infections among a Chinese population: an immunological profile. Infectious Diseases of Poverty, 2(1), 18. [CrossRef] [PubMed] [Google Scholar]
- Tiwari BR, Ghimire P, Malla S, Sharma B, Karki S. 2013. Intestinal parasitic infection among the HIV-infected patients in Nepal. Journal of Infection in Developing Countries, 7(7), 550–555. [CrossRef] [PubMed] [Google Scholar]
- Tuli L, Gulati AK, Sundar S, Mohapatra TM. 2008. Correlation between CD4 counts of HIV patients and enteric protozoan in different seasons – an experience of a tertiary care hospital in Varanasi (India). BMC Gastroenterology, 8, 36. [CrossRef] [PubMed] [Google Scholar]
- Tuli L, Singh DK, Gulati AK, Sundar S, Mohapatra TM. 2010. A multiattribute utility evaluation of different methods for the detection of enteric protozoa causing diarrhea in AIDS patients. BMC Microbiology, 10, 11. [CrossRef] [PubMed] [Google Scholar]
- Tumwine JK, Kekitiinwa A, Bakeera-Kitaka S, Ndeezi G, Downing R, Feng X, Akiyoshi DE, Tzipori S. 2005. Cryptosporidiosis and microsporidiosis in Ugandan children with persistent diarrhea with and without concurrent infection with the human immunodeficiency virus. American Journal of Tropical Medicine and Hygiene, 73(5), 921–925. [CrossRef] [Google Scholar]
- Ukwah BN, Ezeonu IM, Ezeonu CT, Roellig D, Xiao L. 2017. Cryptosporidium species and subtypes in diarrheal children and HIV-infected persons in Ebonyi and Nsukka, Nigeria. Journal of Infection in Developing Countries, 11(2), 173–179. [CrossRef] [PubMed] [Google Scholar]
- UNAIDS. 2017. Fact sheet - Latest global and regional statistics on the status of the AIDS epidemic. [cited 2018, 28 June]; Available from: http://www.unaids.org/sites/default/files/media_asset/UNAIDS_FactSheet_en.pdf. [Google Scholar]
- Uppal B, Kashyap B, Bhalla P. 2009. Enteric pathogens in HIV/AIDS from a tertiary care hospital. Indian Journal of Community Medicine, 34(3), 237–242. [CrossRef] [Google Scholar]
- Uppal B, Singh O, Chadha S, Jha AK. 2014. A comparison of nested PCR assay with conventional techniques for diagnosis of intestinal cryptosporidiosis in AIDS cases from Northern India. Journal of Parasitology Research, 2014, 706105. [CrossRef] [PubMed] [Google Scholar]
- Uysal HK, Adas GT, Atalik K, Altiparmak S, Akgul O, Saribas S, Gurcan M, Yuksel P, Yildirmak T, Kocazeybek B, Ziver T, Oner YA. 2017. The prevalence of Cyclospora cayetanensis and Cryptosporidium spp. in Turkish patients infected with HIV-1. Acta Parasitologica, 62(3), 557–564. [CrossRef] [PubMed] [Google Scholar]
- Vignesh R, Balakrishnan P, Shankar EM, Murugavel KG, Hanas S, Cecelia AJ, Thyagarajan SP, Solomon S, Kumarasamy N. 2007. High proportion of isosporiasis among HIV-infected patients with diarrhea in southern India. American Journal of Tropical Medicine and Hygiene, 77(5), 823–824. [CrossRef] [Google Scholar]
- Vouking MZ, Enoka P, Tamo CV, Tadenfok CN. 2014. Prevalence of intestinal parasites among HIV patients at the Yaounde Central Hospital. Cameroon. Pan African Medical Journal, 18, 136. [Google Scholar]
- Vyas N, Pathan N, Aziz A. 2012. Enteric pathogens in HIV-positive patients with diarrhoea and their correlation with CD4+ T-lymphocyte counts. Tropical Parasitology, 2(1), 29–34. [CrossRef] [PubMed] [Google Scholar]
- Vyas N, Sood S, Sharma B, Kumar M. 2013. The prevalence of intestinal parasitic infestation and the related profile of the CD4 (+) counts in HIV/AIDS people with diarrhoea in Jaipur City. Journal of Clinical and Diagnostic Research, 7(3), 454–456. [Google Scholar]
- Wanachiwanawin D, Chokephaibulkit K, Lertlaituan P, Ongrotchanakun J, Chinabut P, Thakerngpol K. 2002. Intestinal microsporidiosis in HIV-infected children with diarrhea. Southeast Asian Journal of Tropical Medicine and Public Health, 33(2), 241–245. [Google Scholar]
- Wang L, Zhang H, Zhao X, Zhang L, Zhang G, Guo M, Liu L, Feng Y, Xiao L. 2013. Zoonotic Cryptosporidium species and Enterocytozoon bieneusi genotypes in HIV-positive patients on antiretroviral therapy. Journal of Clinical Microbiology, 51(2), 557–563. [CrossRef] [PubMed] [Google Scholar]
- Wang Z-D, Liu Q, Liu H-H, Li S, Zhang L, Zhao Y-K, Zhu X-Q. 2018. Prevalence of Cryptosporidium, microsporidia and Isospora infection in HIV-infected people: a global systematic review and meta-analysis. Parasites & vectors, 11(1), 28. [CrossRef] [PubMed] [Google Scholar]
- Wanyiri JW, Kanyi H, Maina S, Wang DE, Steen A, Ngugi P, Kamau T, Waithera T, O’Connor R, Gachuhi K, Wamae CN, Mwamburi M, Ward HD. 2014. Cryptosporidiosis in HIV/AIDS patients in Kenya: clinical features, epidemiology, molecular characterization and antibody responses. American Journal of Tropical Medicine and Hygiene, 91(2), 319–328. [CrossRef] [Google Scholar]
- Weitzel T, Dittrich S, Möhl I, Adusu E, Jelinek T. 2006. Evaluation of seven commercial antigen detection tests for Giardia and Cryptosporidium in stool samples. Clinical Microbiology and Infection, 12(7), 656–659. [CrossRef] [Google Scholar]
- Werneck-Silva AL, Prado IB. 2009. Gastroduodenal opportunistic infections and dyspepsia in HIV-infected patients in the era of highly active antiretroviral therapy. Journal of Gastroenterology and Hepatology, 24(1), 135–139. [CrossRef] [PubMed] [Google Scholar]
- Wiwanitkit V. 2001. Intestinal parasitic infections in Thai HIV-infected patients with different immunity status. BMC Gastroenterology, 1(1), 3. [CrossRef] [PubMed] [Google Scholar]
- World Bank. World Bank Country and Lending Groups. 2017 [cited 2018/28/6]; Available from: https://datahelpdesk.worldbank.org/knowledgebase/articles/906519. [Google Scholar]
- World Health Organization. 2003. List of Member States by WHO region and mortality stratum. World Health Report, 2003, 182. [Google Scholar]
- Wumba RD, Zanga J, Mbanzulu KM, Mandina MN, Kahindo AK, Aloni MN, Ekila MB. 2015. Cryptosporidium identification in HIV-infected humans. Experience from Kinshasa, the Democratic Republic of Congo. Acta Parasitologica, 60(4), 638–644. [CrossRef] [PubMed] [Google Scholar]
- Xiao L. 2010. Molecular epidemiology of cryptosporidiosis: an update. Experimental parasitology, 124(1), 80–89. [Google Scholar]
- Xiao L, Cama VA. 2018. Cryptosporidium and cryptosporidiosis, in Foodborne parasites. Springer. p. 73–117. [Google Scholar]
- Yang Y, Zhou Y, Cheng W, Pan X, Xiao P, Shi Y, Gao J, Song X, Chen Y, Jiang Q. 2017. Prevalence and determinants of Cryptosporidium infection in an underdeveloped rural region of Southwestern China. American Journal of Tropical Medicine and Hygiene, 96(3), 595–601. [Google Scholar]
- Yang Y, Zhou YB, Xiao PL, Shi Y, Chen Y, Liang S, Yihuo WL, Song XX, Jiang QW. 2017. Prevalence of and risk factors associated with Cryptosporidium infection in an underdeveloped rural community of southwest China. Infectious Diseases of Poverty, 6(1), 2. [CrossRef] [PubMed] [Google Scholar]
- Zaidah AR, Chan YY, Asma HS, Abdullah S, Nurhaslindawati AR, Salleh M, Zeehaida M, Lalitha P, Mustafa M, Ravichandran M. 2008. Detection of Cryptosporidium parvum in HIV-infected patients in Malaysia using a molecular approach. Southeast Asian Journal of Tropical Medicine and Public Health, 39(3), 511–516. [Google Scholar]
- Zali MR, Mehr AJ, Rezaian M, Meamar AR, Vaziri S, Mohraz M. 2004. Prevalence of intestinal parasitic pathogens among HIV-positive individuals in Iran. Japanese Journal of Infectious Diseases, 57(6), 268–270. [PubMed] [Google Scholar]
- Zavvar M, Sadraei J, Emadi H, Pirestani M. 2008. The use of a nested PCR-RFLP technique, based on the parasite’s 18S ribosomal RNA, to characterise Cryptosporidium isolates from HIV/AIDS patients. Annals of Tropical Medicine & Parasitology, 102(7), 597–601. [CrossRef] [Google Scholar]
- Zeynudin A, Hemalatha K, Kannan S. 2013. Prevalence of opportunistic intestinal parasitic infection among HIV infected patients who are taking antiretroviral treatment at Jimma Health Center, Jimma, Ethiopia. European Review for Medical and Pharmacological Sciences, 17(4), 513–516. [PubMed] [Google Scholar]
- Zhang L, Fu Y, Jing W, Xu Q, Zhao W, Feng M, Tachibana H, Sui G, Cheng X. 2015. Rapid microfluidic immunoassay for surveillance and diagnosis of Cryptosporidium infection in human immunodeficiency virus-infected patients. Biomicrofluidics, 9(2), 024114. [PubMed] [Google Scholar]
Cite this article as: Ahmadpour E, Safarpour H, Xiao L, Zarean M, Hatam-Nahavandi K, Barac A, Picot S, Rahimi MT, Rubino S, Mahami-Oskouei M, Spotin A, Nami S & Baghi HB. 2020. Cryptosporidiosis in HIV-positive patients and related risk factors: A systematic review and meta-analysis. Parasite 27, 27.
All Tables
Pooled prevalence of Cryptosporidium in HIV-positive patients and subgroup analyses.
All Figures
 |
Figure 1 Flowchart describing the study design. |
| In the text | |
 |
Figure 2 Forest plot diagram: The estimated pooled prevalence of Cryptosporidium infection in people with HIV infection by random-effect meta-analysis in included studies based on the PCR technique (first author, year of publication, and country). Note: The area of each square is proportional to the study’s weight in the meta-analysis, and each line represents the confidence interval around the estimate. The diamond represents the pooled estimate. |
| In the text | |
 |
Figure 3 Forest plot diagram: The estimated pooled prevalence of Cryptosporidium infection in people with HIV infection by random-effect meta-analysis in included studies based on serological methods (first author, year of publication, and country). Note: The area of each square is proportional to the study’s weight in the meta-analysis, and each line represents the confidence interval around the estimate. The diamond represents the pooled estimate. |
| In the text | |
 |
Figure 4 Forest plot diagram: The estimated pooled prevalence of Cryptosporidium infection in people with HIV infection by random-effect meta-analysis in included studies based on the staining method (first author, year of publication, and country). Note: The area of each square is proportional to the study’s weight in the meta-analysis, and each line represents the confidence interval around the estimate. The diamond represents the pooled estimate. |
| In the text | |
 |
Figure 5 Pooled prevalence of Cryptosporidium in HIV-positive patients in different countries (source of image: https://commons.wikimedia.org/wiki/File:BlankMap-World.svg). |
| In the text | |
 |
Figure 6 Funnel plot of standard error by logit event rate to assess publication or other types of bias across prevalence studies. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


