| Issue |
Parasite
Volume 22, 2015
|
|
|---|---|---|
| Article Number | 30 | |
| Number of page(s) | 4 | |
| DOI | https://doi.org/10.1051/parasite/2015030 | |
| Published online | 29 October 2015 | |
Short Note
Fatal Toxoplasma gondii infection in the giant panda
Infection fatale à Toxoplasma gondii chez le panda géant
大熊猫弓形虫致死性感染
1
College of Life Science, Jilin Agricultural University, 2888 Xincheng Street, Changchun
130118, Jilin Province, China
2
Key Laboratory of Jilin Province for Zoonosis Prevention and Control, Military Veterinary Institute, Academy of Military Medical Sciences, Changchun, China
3
China Conservation and Research Center for the Giant Panda, Ya’an, China
* Corresponding author: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
27
September
2015
Accepted:
15
October
2015
Abstract
Toxoplasma gondii can infect nearly all warm-blooded animals. We report an acute fatal T. gondii infection in the endangered giant panda (Ailuropoda melanoleuca) in a zoo in China, characterized by acute gastroenteritis and respiratory symptoms. T. gondii infection was confirmed by immunological and molecular methods. Multilocus nested PCR-RFLP revealed clonal type I at the SAG1 and c29-2 loci, clonal type II at the SAG2, BTUB, GRA6, c22-8, and L358 loci, and clonal type III at the alternative SAG2 and SAG3 loci, thus, a potential new genotype of T. gondii in the giant panda. Other possible pathogens were not detected. To our knowledge, this is the first report of clinical toxoplasmosis in a giant panda.
Résumé
Toxoplasma gondii peut infecter presque tous les animaux à sang chaud. Nous rapportons une infection fatale aiguë par T. gondii chez le panda géant (Ailuropoda melanoleuca), une espèce en danger, dans un zoo en Chine, caractérisée par une gastro-entérite aiguë et des symptômes respiratoires. L’infection par T. gondii a été confirmée par des méthodes immunologiques et moléculaires. La PCR-RFLP nichée a révélé le type clonal I aux loci SAG1 et c29-2, le type clonal II aux loci SAG2, BtuB, GRA6, c22-8 et L358, le type clonal III aux loci alternatifs SAG2 et SAG3, et donc un nouveau génotype potentiel de T. gondii chez le panda géant. Aucun autre agent pathogène n’a été détecté. À notre connaissance, ceci est le premier signalement de toxoplasmose clinique chez le panda géant.
摘要
弓形虫能感染几乎所有的温血动物。本文报道了一例发生在中国动物园的濒危动物大熊猫急性致死性弓形虫感染病例,其主要临床特征表现为急性胃肠炎和呼吸系统症状。弓形虫感染经免疫学及分子生物学方法确证。多位点巢式PCR限制性片段长度多态性分析表明,感染弓形虫SAG1和c29-2位点为I型,SAG2,BTUB,GRA6,c22-8和L358位点为II型,alternative SAG2和SAG3位点为III型,显示大熊猫感染弓形虫可能为一种新基因型。未检测到可导致性胃肠炎和呼吸系统症状的其它病原体。这是首例大熊猫弓形虫感染病例。
Key words: Toxoplasma gondii / Giant panda / Genotype / PCR
© H. Ma et al., published by EDP Sciences, 2015
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Toxoplasmosis, caused by the obligate intracellular protozoan Toxoplasma gondii, is an important zoonosis worldwide. It is a major public health concern, mainly because of congenital disease, infection of immunocompromised patients, and an emerging severe form of acquired toxoplasmosis in immunocompetent patients [1]. The lifecycle of T. gondii includes sexual multiplication within cats and asexual multiplication within nearly all warm-blooded animals, including humans [6]. Humans and animals become infected by eating undercooked or raw meat containing cysts, or by ingesting food or water contaminated with sporulated oocysts.
The giant panda (Ailuropoda melanoleuca) is an emblematic endangered species and regarded as a national treasure and “living fossil” in China [16]. Its population is estimated at approximately 1600 in the wild, and the captive population is more than 300 [7, 13]. The health of giant pandas has attracted global attention. Here, we report an acute fatal T. gondii infection in the giant panda in China.
Case presentation
In February 2014, a seven-year-old giant panda named Jin Yi was found dead at Zhengzhou Zoo, Henan Province, China. The panda did not eat at noon on February 7. On February 8, the panda was found lying in the room with head buried in the abdomen. Treatment measures included intramuscular administration of cephalosporin and intravenous infusion of glucose. The animal had difficulty breathing overnight and was found dead in the morning of February 9.
A complete necropsy was conducted. Severe pathologic lesions were found, localized to the gastrointestinal tract and lungs. The gastrointestinal tract contained little or no ingesta, had multifocal mucosal hemorrhage, and dry, hard-packed digesta in the duodenum. Lungs were congested and chyme blocked the respiratory tract. Histologically, macrophages containing T. gondii tachyzoites were seen in the alveoli (Fig. 1). Other lesions included congestion in the intestinal lamina propria and submucosa, gastric epithelial necrosis, and sloughing.
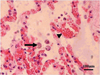 |
Figure 1. Many macrophages containing Toxoplasma gondii tachyzoites (arrow) in the alveoli, and dilated capillaries (arrowhead) in the alveolar wall. Giant panda lung, hematoxylin-eosin stain. |
Serum and tissue samples were collected for examination of potential pathogens that may cause hemorrhagic gastroenteritis. The animal had an antibody titer for T. gondii of 200 by the modified agglutination test [5]. T. gondii DNA was detected in the liver, spleen, lungs, kidneys, and small and large intestines by nested PCR targeting the B1 gene [12]. The immunofluorescence assay (IFA) revealed T. gondii tachyzoites present in the lung and small intestine tissues (Fig. 2), suggesting acute orally acquired toxoplasmosis in the giant panda, probably occurring 7–10 days before signs.
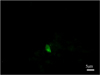 |
Figure 2. Immunofluorescence assay (IFA) conducted on the frozen tissues using monoclonal antibodies against tachyzoite-specific surface antigen SAG1 showing Toxoplasma gondii tachyzoites in the lungs of the giant panda. |
The positive DNA samples were directly typed by multilocus nested PCR-RFLP (Mn-PCR-RFLP) using 10 genetic markers (SAG1, SAG2, SAG3, BTUB, GRA6, c22-8, c29-2, L358, PK1, and Apico), and the reference strains, including GT1, PTG, CTG, MAS, TgCgCa1, TgCatBr5, TgCatBr40, TgCatBr64, and TgRsCr1, were used as positive controls. The results revealed clonal type I at the SAG1 and c29-2 loci, clonal type II at the SAG2, BTUB, GRA6, c22-8, and L358 loci, and clonal type III at the alternative SAG2 and SAG3 loci, showing a potential new atypical genotype of T. gondii in the giant panda. Other potential pathogens, including viruses and bacteria that cause acute gastroenteritis, or respiratory disease, were not detected. These results demonstrated that the giant panda died from acute toxoplasmosis due to a T. gondii strain of an atypical genotype.
Discussion
Toxoplasma gondii is considered to be one of the most successful eukaryotic pathogens, based on the number of host species and percentage of animals infected worldwide. The consequences of infection with T. gondii are associated with the host species and parasite genotypes. Primary infections in adults are mostly asymptomatic, but severe, acute, disseminated toxoplasmosis can occur in immunocompetent hosts when infected with some isolates [11]. Many T. gondii genotypes identified in animals and humans show high genetic diversity of T. gondii in China [10]. In addition to the atypical ToxoDB#9, there are several other atypical T. gondii genotypes identified in animals and humans in China 1 [2, 17, 14]. Atypical T. gondii strains have been shown to cause severe clinical disease in immunocompetent hosts [4, 9].
Despite its taxonomic classification as a carnivore, the giant panda has a diet that is primarily herbivorous, almost exclusively bamboo. The panda still retains decidedly ursine teeth and will eat meat when available [15]. In addition to bamboo, the captive panda is given some formulated biscuits or other dietary supplements. There are a number of stray cats and small rodents in the zoo, and these animals can freely roam in the habitat of the giant panda. The infection may be obtained by consuming food or water contaminated with sporulated oocysts, or by ingestion of rodents infected with T. gondii [3]. Treatment of the disease should include pyrimethamine plus sulfadiazine. Avoiding consumption of raw or undercooked meat is the main measure recommended to prevent T. gondii infection [8].
Acknowledgments
This study was supported financially by the International Cooperative Research Project of the Giant Panda (SD0627), the Special Fund for Agro-Scientific Research in the Public Interest (201303042), and the National Natural Science Foundation of China (31372430). The authors declare that there is no conflict of interest.
References
- Carme B, Demar M, Ajzenberg D, Dardé ML. 2009. Severe acquired toxoplasmosis caused by wild cycle of Toxoplasma gondii, French Guiana. Emerging Infectious Diseases, 15, 656–658. [CrossRef] [PubMed] [Google Scholar]
- Chen ZW, Gao JM, Huo XX, Wang L, Yu L, Halm-Lai F, Xu YH, Song WJ, Hide G, Shen JL, Lun ZR. 2011. Genotyping of Toxoplasma gondii isolates from cats in different geographic regions of China. Veterinary Parasitology, 183, 166–170. [CrossRef] [PubMed] [Google Scholar]
- Elmore SA, Jones JL, Conrad PA, Patton S, Lindsay DS, Dubey JP. 2010. Toxoplasma gondii: epidemiology, feline clinical aspects, and prevention. Trends in Parasitology, 26, 190–196. [CrossRef] [PubMed] [Google Scholar]
- Fernandez-Aguilar X, Ajzenberg D, Cabezon O, Martinez-Lopez A, Darwich L, Dubey JP, Almeria S. 2013. Fatal toxoplasmosis associated with an atypical Toxoplasma gondii strain in a Bennett’s wallaby (Macropus rufogriseus) in Spain. Veterinary Parasitology, 196, 523–527. [CrossRef] [PubMed] [Google Scholar]
- Liu Q, Wang ZD, Huang SY, Zhu XQ. 2015. Diagnosis of toxoplasmosis and typing of Toxoplasma gondii. Parasites & Vectors, 28, 292. [Google Scholar]
- Liu Q, Singla LD, Zhou H. 2012. Vaccines against Toxoplasma gondii: status, challenges and future directions. Human Vaccines & Immunotherapeutics, 8, 1305–1308. [CrossRef] [PubMed] [Google Scholar]
- Liu X, He T, Zhong Z, Zhang H, Wang R, Dong H, Wang C, Li D, Deng J, Peng G, Zhang L. 2013. A new genotype of Cryptosporidium from giant panda (Ailuropoda melanoleuca) in China. Parasitology International, 62, 454–458. [CrossRef] [PubMed] [Google Scholar]
- Montoya JG, Liesenfeld O. 2004. Toxoplasmosis. Lancet, 363, 1965–1976. [CrossRef] [PubMed] [Google Scholar]
- Qian W, Wang H, Su C, Shan D, Cui X, Yang N, Lv C, Liu Q. 2012. Isolation and characterization of Toxoplasma gondii strains from stray cats revealed a single genotype in Beijing, China. Veterinary Parasitology, 187, 408–413. [CrossRef] [PubMed] [Google Scholar]
- Shwab EK, Zhu XQ, Majumdar D, Pena HF, Gennari SM, Dubey JP, Su C. 2014. Geographical patterns of Toxoplasma gondii genetic diversity revealed by multilocus PCR-RFLP genotyping. Parasitology, 141, 453–461. [CrossRef] [PubMed] [Google Scholar]
- Su C, Shwab EK, Zhou P, Zhu XQ, Dubey JP. 2010. Moving towards an integrated approach to molecular detection and identification of Toxoplasma gondii. Parasitology, 137, 1–11. [CrossRef] [PubMed] [Google Scholar]
- Sun H, Wang Y, Zhang Y, Ge W, Zhang F, He B, Li Z, Fan Q, Wang W, Tu C, Li J, Liu Q. 2013. Prevalence and genetic characterization of Toxoplasma gondii in bats in Myanmar. Applied and Environmental Microbiology, 79, 3526–3528. [CrossRef] [PubMed] [Google Scholar]
- Wang Y, Zhao PX. 2012. Habitat assessment of giant panda in Qingmuchuan Nature Reserve, Shaanxi Province of Northwest China. Journal of Applied Ecology, 23, 206–212. [Google Scholar]
- Zhang XX, Huang SY, Zhang YG, Zhang Y, Zhu XQ, Liu Q. 2014. First Report of genotyping of Toxoplasma gondii in free-living Microtus fortis in Northeastern China. Journal of Parasitology, 100, 692–694. [CrossRef] [Google Scholar]
- Zhao H, Yang JR, Xu H, Zhang J. 2010. Pseudogenization of the umami taste receptor gene Tas1r1 in the giant panda coincided with its dietary switch to bamboo. Molecular Biology and Evolution, 27, 2669–2673. [CrossRef] [PubMed] [Google Scholar]
- Zhao S, Zheng P, Dong S, Zhan X, Wu Q, Guo X, Hu Y, He W, Zhang S, Fan W, Zhu L, Li D, Zhang X, Chen Q, Zhang H, Zhang Z, Jin X, Zhang J, Yang H, Wang J, Wang J, Wei F. 2013. Whole-genome sequencing of giant pandas provides insights into demographic history and local adaptation. Nature Genetics, 45, 67–71. [CrossRef] [PubMed] [Google Scholar]
- Zhou P, Nie H, Zhang LX, Wang HY, Yin CC, Su C, Zhu XQ, Zhao JL. 2010. Genetic characterization of Toxoplasma gondii isolates from pigs in China. Journal of Parasitology, 96, 1027–1029. [CrossRef] [Google Scholar]
Cite this article as: Ma H, Wang Z, Wang C, Li C, Wei F & Liu Q: Fatal Toxoplasma gondii infection in the giant panda. Parasite, 2015, 22, 30.
All Figures
 |
Figure 1. Many macrophages containing Toxoplasma gondii tachyzoites (arrow) in the alveoli, and dilated capillaries (arrowhead) in the alveolar wall. Giant panda lung, hematoxylin-eosin stain. |
| In the text | |
 |
Figure 2. Immunofluorescence assay (IFA) conducted on the frozen tissues using monoclonal antibodies against tachyzoite-specific surface antigen SAG1 showing Toxoplasma gondii tachyzoites in the lungs of the giant panda. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


